Wrists
Carpal Tunnel Syndrome
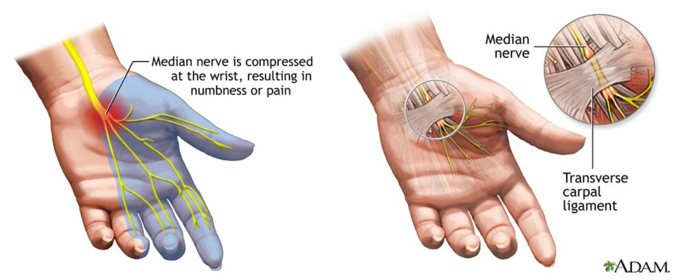
The carpal tunnel is a narrow passageway located in the anterior wrist bounded by a row of carpal bones forming the floor of the tunnel, and the flexor retinaculum forming the roof. This tunnel has just enough room for the soft tissue tendons, nerves and blood vessels that pass through it into the hand. Anything that causes a reduction in the space in the tunnel will cause pressure on the nerve and blood vessels causing pain, pins and needles and numbness into the hand.
Causes of carpal tunnel syndrome
What can cause a reduction in the space? There are a multitude of factors which can cause carpal tunnel such as:
- Swelling of the tendons due to repetitive use,
- Fluid retention during pregnancy or menopause,
- Arthritis causing bony spurs which may cause an impingement,
- An injury to the wrist or lower arm,
- Tendonitis
- A cyst or tumour in the narrow tunnel,
- Diabetes,
- Hypothyroidism
This may happen in one hand or both hands. Sometimes carpal tunnel occurs without reason.
How carpal tunnel presents
Commonly patients presenting to the clinic with carpal tunnel syndrome will have the following:
- tingling or numbness in the thumb, index and middle fingers fingers,
- neuropathic pain predominantly in the wrist, hand, thumb and fingers but sometimes also in the lower arm,
- weakness in the hands, especially when gripping objects,
- visible wasting of the muscles in the palm which are supplied by the median nerve, and
- swollen fingers.
Management
Treatment and ongoing management of carpal tunnel depends on its cause. Initially other structures such as the cervical spine, need to be ruled out as pain referral sites.
Treatment options can include:
- Wearing a wrist splint form fitted for your wrist to keep the wrist in a neutral position (especially at night) and relieve pressure on the median nerve,
- aggravating activity avoidance or at the very least, activity modification,
- ice, elevation, soft tissue techniques,
- physiotherapy techniques such as taping, deep tissue release, forearm stretches and gentle eccentric strengthening exercises,
- anti-inflammatory medicines to ease pain
If the patient is not responding to the above options, the following can be investigated:
- corticosteroid injections into the wrist, and
- surgery - carpal tunnel release
If you think you may have carpal tunnel syndrome, or are experiencing some of the symptoms listed here, book an appointment today. Outcomes are better if management is commenced sooner rather than later.
Colles Fracture
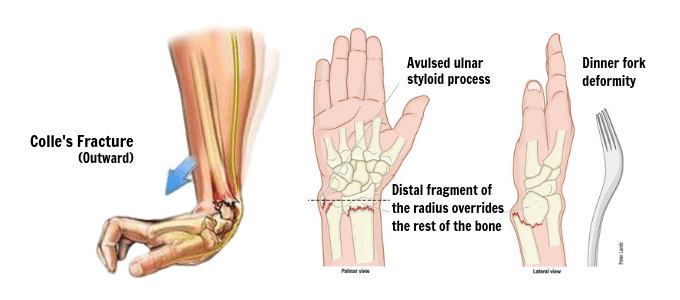
The most common wrist fracture occurs in the distal, (furthest end) of the radius. The radius is the larger of the two forearm bones. Most commonly, this fracture occurs when a patient has fallen on their outstretched arm.
How does a Colles fracture occur?
'FOOSH' or 'fall onto an outstretched hand' is a mechanism of injury associated with a traumatic event occurring when an individual falls. In an attempt to protect themselves, they land heavily on the palm, transferring energy through the long axis of the radius, which fails and breaks.
This type of fracture is common in horse riding where riders are thrown off their horse, skiing and snowboarding, bicycle accidents, car accidents and any other activities that will cause an individual to try and break their fall.
Management
Initial management of a Colles fracture is dependent on many factors such as the severity and position of the fracture, a patient's age and their activity level.
If the fractured bone is well positioned, a cast is applied for a period until the bone heals. However, if the alignment of the bone is poor, a realignment procedure will be performed, and dependent on the severity of the displacement, a reduction can either be closed - without surgery, or open - with surgery.
Physiotherapy management is focused on gently regaining movement and strength following the period of immobilisation.

Tendonitis
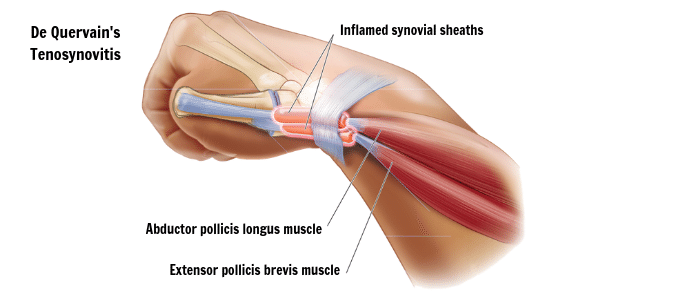
Tendonitis, or tenosynovitis is very common, due to location, anatomy and the repetitive nature of tasks performed by the hand and wrist.
There are a number of tendons crossing the wrist that can become symptomatic, the:
- common extensor tendons,
- common flexor tendons, and
- the tendons acting on the thumb.
Symptoms of wrist tendonitis
The most common and consistent complaint of patients diagnosed with wrist tendonitis is pain in the wrist. Other symptoms of wrist tendonitis include:
- swelling in and around the joint,
- warmth and redness, and
- crepitus - a grinding sensation on movement of the tendons.
Management
As with the majority of inflammatory conditions, management needs to commence with avoidance of the aggravating activity and a period of immobilisation to allow the tendons to rest and heal.
Ice therapy can be useful in reducing inflammation and stimulating blood flow to the general area. NSAIDS can also be effective if combined with a period of rest.
Physiotherapy management can include gentle stretching of the tendons and surrounding musculature, strengthening and progressive custom fit splints to control movement.
In some instances, a cortisone injection into the area +/- surgical intervention can be beneficial if conservative measures have failed to resolve the condition.